If you or your loved ones live with diabetes or have noticed changes in your vision, it is strongly recommended to schedule a comprehensive diabetic eye screening. This allows the specialist to identify the cause and detect any early signs of diabetic eye disease before vision is affected.
This blog on upper blepharoplasty has been contributed by Dr. Alia Issa, Aesthetic Oculoplastic Surgeon at Moorfields Eye Hospital Dubai
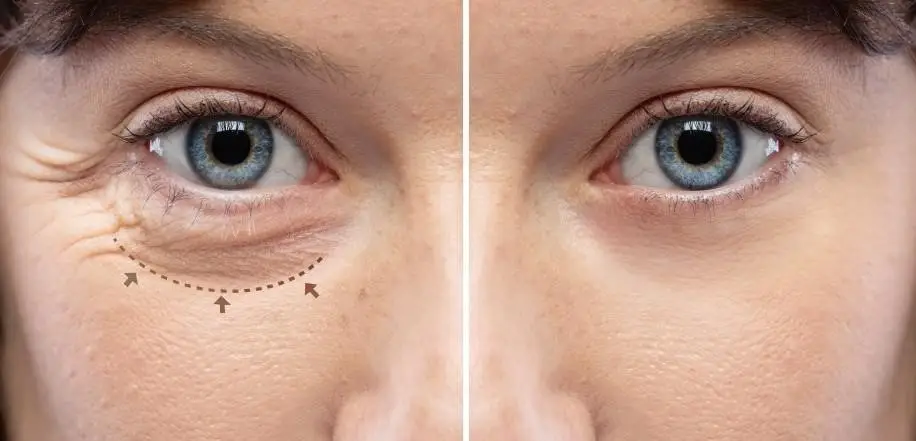
Upper blepharoplasty is a common eyelid rejuvenation procedure for individuals who have droopy eyelids or tired-looking eyes. While it is often seen as removal of excess skin, the factors involved in the procedure are far more complex. There are several deeper anatomical structures that influence how the eyelids look and function, and understanding these is essential for achieving natural, healthy, and desired results.
Whether you are exploring blepharoplasty or seeking clarity after receiving varied advice, this blog provides an understanding of the procedure and factors involved.
What are the reasons behind droopy or saggy eyelids?
The upper eyelids are one of the first areas of the face to show signs of ageing. Fine skin, expressive muscles, shifting fat, and the influence of the brows all contribute to the overall appearance. These changes often happen gradually and differently on each side, which can make the eyes look asymmetrical or tired.
Upper blepharoplasty aims to restore a more refreshed appearance, but only when all contributing factors are assessed, not only the excess skin. Our oculoplastic surgeons evaluate the deeper structures around the eyes to support both appearance and long-term eyelid health.
Below are the factors examined during consultation to support an effective and natural blepharoplasty outcome.
1. The brow position is often a hidden cause of droopy eyelids
The brow significantly influences the appearance of the eyelid, often more than most people expect. As we age, the outer part of the brow gradually drifts downward. When this happens, it pushes skin and soft tissue onto the upper eyelid, creating the impression of excess skin or heaviness, even when actual excess skin is minimal.
If a surgeon removes eyelid skin without evaluating the brow position, the result may appear tight, unbalanced, or may not lift the heaviness as expected. In some cases, removing skin alone can even make the brow descent more noticeable.
This is why each consultation should include assessing the brow height, shape, and symmetry before planning any blepharoplasty. This helps determine whether the brow is contributing to the overall heaviness and ensures the eyelid is not over-corrected.
2. Determining the right amount of skin to remove
Even when excess skin is present, the goal is a careful and conservative approach. The eyelids protect the eye’s surface, maintain healthy blinking, and support a smooth tear film. Removing too much skin may make eyelid closure difficult and lead to dryness or discomfort, while removing too little may not achieve the desired result.
Our oculoplastic surgeons examine:
- The natural crease height,
- Elasticity of the skin,
- The relationship between the lid and brow,
- Symmetry between both eyes,
- Blink mechanics.
This ensures that any skin removal enhances the appearance without compromising function, especially important in a climate like Dubai, where air-conditioning can intensify dry eye symptoms.
3. Fat distribution
Ageing affects the fat around the eyes in different ways. In some areas, fat may protrude forward, creating puffiness. In others, fat may diminish, causing a hollow, tired look. These changes vary between individuals and often between the two eyes.
If fat prolapse or hollowing is not addressed during surgery, the result may appear uneven or prematurely aged. Therefore, the oculoplastic surgeon will evaluate the fat prolapse carefully, deciding whether to:
- Reduce prolapsed fat,
- preserve fat to maintain youthful volume,
- or subtly reposition fat to balance the contours.
This personalised approach prevents hollowing or over-correction, helping maintain a natural and well-rested appearance.
4. Eyelid height, muscle function and ptosis
In some individuals, the muscle that lifts the eyelid (the levator muscle) can weaken over time. When this happens, the upper eyelid sits lower than it should leading to a condition known as ptosis. Ptosis often goes unnoticed by patients until it is pointed out, yet it significantly influences how alert or tired the eyes appear.
If ptosis is not identified before surgery, simply removing skin will not correct eyelid height. In fact, the tired appearance may persist even after blepharoplasty.
The eyelid height, strength of the lifting muscle, and symmetry must always be evaluated and If ptosis is contributing to the appearance, it may be corrected at the same time as the blepharoplasty for a more natural and youthful result.
5. Tear gland stability
The lacrimal (tear) gland sits in the outer part of the upper eyelid. With age or natural loosening of the supporting tissues, it may shift forward, creating a small bulge. This fullness is often mistaken for fat prolapse or excess skin, but removing skin alone will not improve it.
If the tear gland is not properly addressed, the bulge will remain after surgery. During the pre-operative examination, the surgeon checks whether the gland has prolapsed and, if needed, gently repositions it to support a smooth and natural contour.
Who is upper blepharoplasty suitable for?
You may be a good candidate if you experience:
- droopy or heavy upper eyelids
- puffiness or fullness
- tired-looking eyes
- asymmetry between the eyes
- the desire for a refreshed appearance while maintaining natural expression
A consultation is essential to determine whether excess skin, brow position, ptosis, or fat redistribution is the primary cause.
What can you expect during your blepharoplasty journey consultation?
Your surgeon will examine all five anatomical factors, discuss your goals, take clinical photographs, assess tear function, and create a tailored plan.
- Procedure: Upper blepharoplasty is typically a day procedure under local anaesthesia, with or without sedation. The incision sits in the natural lid crease, allowing the scar to blend seamlessly.
- Recovery: Swelling and bruising are normal in the first 7–10 days. Most daily activities can resume early, while full refinement continues over several weeks.
- Long-term results: When deeper anatomical contributors are addressed, the outcome appears refreshed, symmetric, and naturally expressive, avoiding the hollow or “over-pulled” look sometimes associated with poorly planned surgery.
Recovery and Risks considerations
Every patient heals differently. It is normal for:
- each eye to heal at a slightly different pace
- swelling to take a few weeks to settle
- the eyelids to feel tight initially
- the final refined result can take up-to take 6 months
Results typically last many years, although natural ageing continues
Upper blepharoplasty is generally a low-risk procedure when performed by a trained oculoplastic surgeon. However, like any surgery, it carries potential risks.
These may include:
- temporary bruising or swelling
- temporary dryness or irritation
- asymmetry during the healing phase
- scarring in the eyelid crease
- rare bleeding or infection
- very rare difficulty closing the eyelids if too much skin is removed
- Temporary numbness around the scar and lash line
Your surgeon will explain these risks and guide you through how they are minimised.
Why should blepharoplasty be performed by an oculoplastic surgeon?
Upper blepharoplasty is a cosmetic and functional procedure that affects both appearance and eye health. The eyelids protect the eyes, maintain moisture, support vision, and express emotion. Poor technique or incomplete assessment can lead to dryness, asymmetry, hollowing, or difficulty closing the eyes.
For this reason, the safest and most effective approach is to have the procedure performed by oculoplastic surgeons, who are ophthalmologists with additional specialised training in eyelid and cosmetic surgery.
This matters because:
- Oculoplastic surgeons understand both the cosmetic and functional aspects of eyelids.
- They are trained to protect the eye, the tear film, and surrounding structures.
- They can identify issues such as ptosis, dry eye risk, or tear gland prolapse which are conditions that non-ophthalmic surgeons may overlook.
- They prioritise visual comfort and eyelid function in addition to aesthetics, which reduces the risk of eye anatomy complications.
With the right assessment and expertise, the result can restore a natural, refreshed, and balanced appearance.
FREQUENTLY ASKED QUESTIONS (FAQs)
Will upper blepharoplasty change the shape of my eyes?
Upper blepharoplasty is designed to rejuvenate the upper eyelids rather than change your natural eye shape. When performed by an experienced oculoplastic surgeon, the procedure follows your existing anatomical contours and focuses on reducing heaviness, improving definition, and restoring balance. The aim is to preserve your natural expression while creating a refreshed, well-rested appearance.
Is the scar from an upper blepharoplasty visible?
The incision is carefully placed within the natural upper eyelid crease, allowing it to blend with the surrounding skin as it heals. In the first few weeks, it may appear slightly pink or raised, but this gradually settles. With time and proper healing, the line becomes faint and often barely noticeable, even when the eyes are closed. Makeup can help conceal the area during the initial healing period.
How long do the results last?
While the ageing process continues naturally, most individuals enjoy the benefits of upper blepharoplasty for many years. Because the procedure addresses deeper anatomical factors such as brow position, fat changes and muscle function rather than just surface-level skin, the results tend to age more gracefully. Lifestyle factors, genetics, and skin quality all play a role in longevity, but improvements are generally long-lasting.
Can blepharoplasty help with vision problems caused by droopy eyelids?
If excess upper eyelid skin hangs over the lash line or reduces the upper field of vision, upper blepharoplasty can alleviate this obstruction and improve vision. During your consultation, the surgeon will assess your eyelid anatomy and visual fields to determine whether functional improvement applies in your case.
Am I too young or too old for this procedure?
There is no strict age limit for upper blepharoplasty. Some individuals develop early genetically inherited hooding, while others experience age-related changes much later. Suitability is determined by eyelid anatomy, skin quality, brow position, and general health, not age alone. A detailed assessment will help determine whether the procedure is appropriate for you.
Will I look “different” after surgery?
The intention of upper blepharoplasty is to create a subtle, refreshed appearance rather than a dramatic change. You should still look like yourself, simply more open and rested around the eyes. A well-planned procedure respects your natural proportions and avoids the “surprised” or “pulled” appearance associated with overcorrection.
What happens if I have asymmetry?
Most people have natural differences between their eyes and brows. While blepharoplasty cannot create perfect symmetry, which rarely exists in nature, an experienced oculoplastic surgeon can significantly improve balance by tailoring the approach for each eye.
Every November, Diabetes Awareness Month reminds us that awareness and early prevention can make a lasting difference in living well with diabetes. This year’s World Diabetes Day theme, “Know More, Do More for Diabetes at Work,” highlights how diabetes management extends beyond medical care, shaping our everyday habits, especially in the workplace.
For many people working in Dubai and across the UAE, where long hours and digital screen use are common, understanding how diabetes affects eye health is essential to maintaining well-being and productivity.
This blog explores the connection between diabetes and vision, early signs to watch for, and simple lifestyle choices that can help protect your eyesight, at work and beyond.
Facts about diabetes
According to the International Diabetes Federation (IDF), an estimated 589 million adults worldwide are currently living with diabetes, and the number is projected to reach 853 million by 2050. This global rise reflects changing lifestyles, dietary habits, and reduced physical activity, all contributing to the growing public health challenge of diabetes.
In the United Arab Emirates, around 20.7% of adults aged 20 and above, equivalent to roughly 1.3 million people, are living with diabetes, and this is projected to increase, reaching approximately 23% of the population by 2050 (International Diabetes Federation)
These figures highlight the urgency of early detection and ongoing management to reduce health complications and protect long-term vision and overall well-being.
Diabetes and the working population
According to the International Diabetes Federation, 7 in 10 people living with diabetes are of working age (20–64 years). Maintaining healthy vision can be challenging for busy professionals in the UAE, where modern work often involves long hours at the workplace, extended screen time, and imbalanced diet.
Fluctuating glucose levels can temporarily blur vision, making it difficult to focus, read, or drive. Over time, inconsistent control can damage the retina, impacting vision and workplace performance.
Recognising early signs and adopting preventive habits can help you maintain sharper, more comfortable vision and ensuring that diabetes does not stand in the way of a productive working life.
The link between diabetes and vision
While diabetes is well known for affecting overall health, many people are unaware of its impact on the eyes. Over time, persistently high blood sugar levels can damage the blood vessels in the retina, the light-sensitive tissue at the back of the eye, leading to diabetic retinopathy, one of the leading causes of preventable sight loss worldwide.
The scale of this impact is significant, with the International Agency for the Prevention of Blindness (IAPB) reporting that around one in three people living with diabetes will experience vision complications during their lifetime, and one in ten will develop vision-threatening conditions such as proliferative retinopathy or diabetic macular oedema.
Beyond diabetic retinopathy, diabetes can also increase the risk of other eye conditions, including:
- Cataracts, a condition that causes cloudy or blurred vision and tends to develop earlier in people with diabetes.
- Glaucoma, a group of eye diseases that damage the optic nerve, often without noticeable initial symptoms, can lead to irreversible vision loss.
These conditions often progress silently in their early stages, meaning vision changes may only become apparent once the disease has advanced. Early warning signs can include blurred or fluctuating vision, poor night vision, or seeing dark spots, which should never be ignored. The most effective way to protect eyesight is through regular, comprehensive eye examinations, which enable ophthalmologists to detect early changes and manage complications before they affect sight.
Therefore, understanding these risks is the first step towards prevention, especially for those balancing demanding work schedules and daily routines that can make it challenging to prioritise regular eye care.
Eye health and well-being at work
Managing diabetes at work requires adopting habits that support long-term health. These include:
Eat balanced, low-glycaemic meals:
Choose foods that stabilise blood sugar, such as whole grains, vegetables, lean proteins, and low-glycaemic options, which provide steady energy and reduce sugar spikes. Keep eye-friendly snacks like nuts, fruit, and carrot sticks nearby as they contain vitamins E and A, which are beneficial for eye health.
Stay hydrated
Dehydration can raise blood sugar levels and worsen dry eyes, a common complaint among office workers in Dubai due to highly air-conditioned indoor spaces. Always have a bottle of water and drink regularly throughout the day.
Monitor blood pressure and cholesterol.
Both high blood pressure and elevated cholesterol can accelerate the progression of diabetes-related eye disease. Staying physically active, managing stress, and following your doctor’s recommendations all play a vital role in protecting long-term eye health and preventing complications.
Move regularly
Short, frequent breaks throughout the day help regulate blood sugar, improve circulation, and ease muscle tension. Even brief stretches or short walks during work can make a meaningful difference to overall wellbeing and give your eyes a chance to rest, reducing visual fatigue from prolonged screen time.
Schedule regular eye checks.
An annual comprehensive eye examination is one of the most effective ways to protect your sight. Modern retinal imaging enables ophthalmologists to identify very early changes in the eye, often before any symptoms appear, so they can intervene promptly, prevent further damage, and tailor a treatment plan to your individual needs.
The power of awareness and prevention
According to the International Diabetes Foundation and IAPB, up to 95 per cent of vision loss caused by diabetic retinopathy can be prevented through early detection and timely treatment. Eye screenings should be part of every diabetes care routine, even when vision feels normal.
Prevention always remains the best approach, and consistent blood-sugar control, balanced nutrition, and regular medical follow-up significantly reduce the risk of vision-related complications.
To learn more about diabetic retinopathy, including symptoms, causes, and treatment options, visit https://moorfields.ae/service/retina/diabetic-retinopathy/
Frequently Asked Questions
How often should people with diabetes have an eye exam?
People with diabetes should undergo a comprehensive eye examination at least once every 12 months, even if their vision seems stable. During this exam, the ophthalmologist will assess the retina, optic nerve, and blood vessels using advanced imaging techniques to detect early invisible changes to the naked eye.
Those who already show early signs of diabetic retinopathy or macular changes may be advised to attend check-ups more frequently, sometimes every six months or as their specialist recommends. Regular screening ensures that any progression of eye disease can be managed promptly, significantly reducing the risk of vision loss.
What are the early signs of diabetic eye disease?
In its early stages, diabetic eye disease often develops silently, without noticeable symptoms. However, as the condition progresses, warning signs may include:
- Blurred or fluctuating vision that comes and goes.
- Dark spots, floaters, or shadows in your field of vision.
- Reduced night or colour vision.
- Difficulty focusing on near or distant objects.
Any sudden change in vision should be considered a warning sign. Seeking prompt evaluation from an eye specialist can help detect whether these changes are linked to diabetic retinopathy, cataracts, or another underlying issue. Early diagnosis allows for timely treatment before permanent damage occurs.
Can stable blood sugar really prevent eye disease?
Yes. Keeping blood sugar levels within a healthy range is one of the most effective ways to protect your eyes. Stable blood glucose, blood pressure, and cholesterol help maintain the health of the tiny blood vessels that nourish the retina.
Fluctuating or consistently high blood sugar can cause these vessels to swell, leak, or close off, leading to diabetic retinopathy. Over time, this may result in blurred vision or vision loss. By following a balanced diet, taking prescribed medication, exercising regularly, and monitoring blood glucose as advised by your doctor, you can significantly reduce the risk of developing sight-threatening complications such as diabetic retinopathy and cataracts.
Is vision loss from diabetes reversible?
The reversibility of vision loss depends on how early the condition is detected and treated. In its early stages, diabetic eye disease can often be managed successfully, with treatments such as laser therapy or intravitreal injections helping to stabilise or even improve vision.
However, the vision loss may become irreversible if the disease progresses to an advanced stage where significant damage has occurred (particularly to the retina or optic nerve). This is why early detection through regular eye screenings is so vital. Preventive care, timely diagnosis, and adherence to treatment plans offer the best chance of preserving clear sight for the long term.
How can workplaces support employees with diabetes?
Workplaces play a key role in supporting employees with chronic health conditions such as diabetes. A health-conscious environment can help individuals manage their conditions effectively while maintaining productivity.
Employers can:
- Encourage healthy meal and snack options in cafeterias or vending areas.
- Allow flexible scheduling for medical appointments or eye check-ups.
- Promote regular breaks during long periods of screen use to reduce eye strain and regulate blood sugar.
- Offer wellness initiatives that include diabetes awareness sessions or vision screening days.
Such measures not only support employees’ wellbeing but also improve morale, reduce absenteeism, and enhance overall workplace efficiency. A culture that values health ultimately benefits both staff and organisation alike
Every October, the world comes together to mark World Sight Day, a global initiative led by the International Agency for the Prevention of Blindness (IAPB) to raise awareness about the importance of eye health. World Sight Day falls on 9 October this year under the global overarching theme “Love Your Eyes.”
This year, the focus is “Love Your Eyes at Work,” highlighting that protecting our vision is essential for personal well-being, productivity, and safety in the workplace.
Whether you spend your day in front of a computer, driving long distances, teaching, or working outdoors, your eyes are constantly at work. Yet, they are often overlooked in workplace health and wellness conversations.
In this blog, we highlight important facts, the importance of eye health in the workplace, the risks you may face, and practical steps to protect your sight for years to come.
General facts about vision and eye health
Globally, at least 2.2 billion people have near or distance vision impairment, and in at least 1 billion of these cases, the impairment could have been prevented or is yet to be addressed (World Health Organisation). The leading causes of vision impairment and blindness are:
The encouraging news is that 90% of all sight loss is preventable or treatable (IAPB). With early detection, most eye diseases can be managed, treated, or their progression slowed.
The importance of eye health at work
Vision problems affect overall quality of life, from daily comfort to productivity, concentration, and safety at work. In 2020, an estimated 143 million working-age adults had moderate or severe vision impairment.
- Good vision improves productivity by 22%. Something as simple as wearing the correct spectacles can significantly enhance work performance.
- Even mild vision impairment can reduce productivity by 10% and accuracy by 22%.
In Dubai and across the UAE, where long working hours, screen-based jobs, and exposure to dust, air conditioning, and intense sunlight are common, protecting eye health in the workplace is more important than ever.
Common workplace eye health issues and solutions
Digital eye strain and dry eyes
Many professionals in the UAE spend 6–10 hours daily on digital devices, which can lead to digital eye strain, blurred vision, headaches, and tired eyes.
Another common issue is dry eye, which occurs because we blink less when using screens, combined with the effects of air-conditioned indoor environments and the region’s hot climate.
Tips to reduce strain and dryness:
- Follow the 20-20-20 rule – every 20 minutes, look at something 20 feet away for at least 20 seconds.
- Use lubricating drops if advised by an eye specialist.
- Stay hydrated and ensure healthy humidity levels indoors.
- Prioritise rest and adequate sleep, as fatigue can worsen digital strain.
The five-minute check
Simple adjustments at your desk can make a big difference. Use this quick Five-Minute Check (IAPB) to optimise your workspace and protect your eyes while working at a screen.
- My chair supports my entire body, and my feet are adequately rested on the floor.
- My monitor is slightly below eye level, helping my eyes to look downward. Note that the recommended placement is 15–20 degrees below eye level.
- My screen is 50–66 cm away from my eyes.
- My screen can tilt and swivel and has inbuilt glare filters.
- My screen is tilted 10° to 20° away from me.
- My screen is positioned away from glare of any lighting or windows.
- My room is well lit.
- My screen is dust free.
- My blue light glasses are within reach.
- I have increased fonts and zoomed in to avoid bending or moving closer to my screen.
Nutrition and healthy eating at work
Eye health starts from within and a diet rich in antioxidants, vitamins, and omega-3 fatty acids can help reduce the risk of age-related eye conditions.
Smart workplace choices:
- Snack on carrots, cucumbers, nuts, and seeds instead of processed foods.
- Add green leafy vegetables, citrus fruits, and oily fish such as salmon to meals.
- Limit excess sugar and refined carbs, particularly if you have diabetes
Protecting your eyes in different work environments
Office workers
- Use the 5-minute checklist.
- Apply the 20-20-20 rule.
- Ensure pro-per lighting to reduce glare.
Outdoor workers
- Wear 100% UV-blocking sunglasses.
- Use protective eyewear against dust, chemicals, or construction debris.
- Take breaks in shaded areas to reduce glare and dryness.
Drivers and pilots
- Keep windscreens clean to minimise glare.
- Divert air conditioning away from blowing directly into your eyes
- Regularly update your prescription glasses or lenses.
- Avoid driving with untreated cataracts, which cause halos and blur.
How to “Love Your Eyes at Work” every day
Building small, consistent habits into your daily routine can help you look after your eyes. Regular eye checks are one of the most important steps you can take.
- Schedule regular eye checks – Early detection of cataract, glaucoma, or diabetic eye disease is crucial in preserving vision.
- Consult a specialist early – Do not ignore redness, discomfort, or blurred vision.
- Follow advice – Apply the steps highlighted to maintain proper eye health.
Eye health is essential for work and life
World Sight Day 2025 calls us to “Love Your Eyes at Work.” Vision is one of our most valuable assets, shaping how we learn, connect, and thrive professionally and personally. By taking proactive steps, you can protect your vision well into the future.
If you are due for an eye check or have noticed any changes in your vision, ensure to take action.
Frequently Asked Questions
How often should i get my eyes checked?
For most adults, a comprehensive eye examination every one to two years is sufficient to maintain healthy vision. However, if your job requires prolonged computer use or you spend much of the day on digital devices, more frequent checks may be beneficial.
Regular eye tests are not just about updating your glasses prescription. They allow ophthalmologists to detect early signs of eye conditions such as glaucoma, cataracts, or retinal disease, many of which may not show obvious symptoms in their initial stages. For individuals living with diabetes, annual eye examinations are essential, as changes to the retina can occur silently and only be detected through professional assessment.
Are dry eyes a serious condition or just a minor discomfort?
Dry eyes are often underestimated as a simple irritation, but they can significantly affect daily comfort, productivity, and even long-term vision. The condition occurs when the eyes do not produce enough tears or when tears evaporate too quickly, often due to prolonged screen use, air-conditioned offices, or environmental factors such as dust and heat.
If left untreated, chronic dry eye can cause inflammation, blurred vision, difficulty focusing, and, in severe cases, damage to the corneal surface. This can interfere with daily tasks, including reading, driving, and computer work.
Dry eye can usually be managed effectively with lifestyle changes, artificial tears, and, when necessary, advanced clinical treatments. Seeking advice early makes a significant difference, helping you maintain comfort at work and avoid complications later in life.
Can workplace habits really affect the development of cataracts?
Cataracts develop naturally with age, but certain lifestyle and occupational factors can influence how quickly they progress. Prolonged exposure to UV light, common among outdoor workers in the UAE, can accelerate cataract formation. Similarly, poor dietary habits, smoking, and not wearing protective eyewear in hazardous environments may also contribute.
Symptoms of cataracts include blurred or cloudy vision, difficulty seeing in low light, or glare around lights, all of which can make workplace tasks more challenging. By protecting your eyes with UV-blocking sunglasses, maintaining a healthy lifestyle, and attending routine eye examinations, you can slow the progression of cataracts and ensure timely treatment if they develop
What is the link between diabetes and vision at work?
Diabetes is one of the leading causes of preventable vision loss worldwide. High blood sugar levels can damage the delicate blood vessels in the retina, leading to a condition called diabetic retinopathy. In its early stages, this condition is usually silent, showing no obvious symptoms. By the time vision changes are noticed, damage may already be advanced.
For working professionals in Dubai and the wider UAE where the prevalence of diabetes is among the highest globally, this poses a significant risk. Reduced vision can impact work performance, safety, and independence.
The most effective protection is regular diabetic eye screening, combined with good blood sugar, blood pressure, and cholesterol control. Early detection allows for treatment options, such as laser therapy or advanced medications, which can preserve sight and help individuals continue performing effectively at work.
What foods should I keep at my desk for healthy eyes?
Nutrition plays a surprisingly powerful role in protecting your eyes at work. Keeping the right snacks at your desk can support eye health, improve concentration, and reduce fatigue.
- Nuts and seeds (such as almonds, walnuts, and sunflower seeds) provide vitamin E and omega-3 fatty acids, which help protect against age-related macular degeneration and dry eyes.
- Fresh fruit such as oranges, berries, and kiwi are rich in vitamin C, an antioxidant that supports the health of blood vessels in the eye.
- Vegetables like carrots, cucumbers, and bell peppers contain beta-carotene and other essential nutrients that contribute to retinal health.
- Fatty fish (ideal for lunch rather than a snack) such as salmon or sardines provide high levels of omega-3, which supports tear film stability and reduces the risk of dry eyes.
By choosing these healthy snacks instead of processed foods high in sugar and refined carbohydrates, you can give your eyes the nutrients they need to perform well throughout the day and safeguard your long-term vision
For many people, reading, working on a laptop, or scrolling on a phone feels effortless. However, when the eyes cannot work together properly at close range, even simple tasks can become uncomfortable and tiring. This can be caused by a condition known as convergence insufficiency, which affects how the eyes align and coordinate, rather than how clearly they see.
In this blog, we explain what convergence insufficiency is, highlight its causes and outline the most effective treatment options available.
What is Convergence Insufficiency?
Convergence insufficiency (CI) is a binocular vision issue where the eyes do not function properly together while focusing on close objects. This lack of coordination means that the eyes have difficulty converging (turning inward) to look at something up close. As a result, individuals may experience symptoms such as double vision, headaches, eye strain, and difficulty reading.
Unlike conditions that affect visual clarity, such as short-sightedness or long-sightedness, Convergence insufficiency affects how the eyes align and move together. Importantly, people with perfect eyesight may still suffer from convergence insufficiency.
This condition is especially common among school-aged children and adolescents, though it can also affect adults, particularly those who spend long hours working at a desk or using digital devices.
The importance of convergence for clear vision
Convergence is essential for activities that involve near vision such as reading and writing. When the eyes cannot maintain proper alignment, the brain receives conflicting visual information. This often results in visual discomfort and can affect concentration and learning ability.
In an era where technology use is high and digital learning is increasingly integrated into the school curriculum, it is particularly important to be aware of how convergence issues may be affecting children’s academic performance and comfort.
Causes of convergence insufficiency
The causes of convergence insufficiency are not always clear, but several factors can contribute to its development:
- Weakness in the eye muscles responsible for convergence
- Poor coordination between the eyes due to neurological factors
- Stress, fatigue, and prolonged screen use may exacerbate symptoms
- Head trauma or concussion, especially in adults or teenagers
It is worth noting that convergence insufficiency is not a result of poor eyesight or the need for glasses, although it may coexist with other vision problems.
Risk factors of Convergence Insufficiency
While the condition can affect anyone, some individuals are at higher risk, including:
- Children and teenagers, particularly those who are doing large amounts of reading or digital work
- Individuals and professionals who work for long periods on digital screens
- Individuals recovering from neurological events such as a concussion or brain injury
- Those experiencing chronic fatigue or visual stress
Convergence insufficiency is often an underdiagnosed condition, especially in children who may not be able to describe what they are seeing as they may assume their symptoms are normal because they may have had it for a long time. However, signs such as being inattentive in school or struggling academically provide clues that a child needs a comprehensive eye exam to check for any vision problems they may be experiencing.
Common signs and symptoms of Convergence Insufficiency
Convergence insufficiency impacts the eyes’ ability to align, and therefore, symptoms often become apparent during or after close-up tasks. These may include:
- Headaches or discomfort around the eyes during or after reading, screen time or other prolonged near tasks
- Double vision when focusing on near objects
- Blurred vision during near tasks
- Difficulty concentrating when reading
- Words appearing to move or jump on the page
- Losing place while reading or skipping lines
- Eye fatigue or strain
- Frequently closing or covering one eye to improve clarity
In children, these symptoms may lead to academic difficulties, frustration, and avoidance of reading. In adults, they may result in reduced productivity, visual discomfort, and mental fatigue, especially during long working hours.
Diagnosing Convergence Insufficiency
Convergence insufficiency is diagnosed through a comprehensive eye examination that includes a series of binocular vision tests with our Ophthalmologists and Orthoptists. These assessments are designed to evaluate how well the eyes work together and include:
- Near point of convergence (NPC) testing: Measures how close the eyes can converge
- Positive fusional vergence testing: Assesses the eyes’ ability to maintain alignment
- Cover test : Observes how the eyes align when switching focus
- Evaluation of eye movements, tracking, and visual endurance
This comprehensive evaluation helps rule out the presence of other eye conditions and ensures that the diagnosis is accurate.
Treatment options for Convergence Insufficiency
Convergence insufficiency is highly treatable condition and most patients respond well to therapy, especially when treatment begins early. At Moorfields Eye Hospital Dubai, our specialists offer several effective management options tailored to each patient.
Vision therapy (Orthoptic exercises)
Vision therapy is the most recommended and evidence-based treatment for convergence insufficiency. This series of eye exercises helps train the brain and eyes coordinate more effectively at near distances. This includes:
- Smooth convergence
- Jump convergence
- Dot card method
- Stereograms
Therapy is usually conducted In-clinic, under the guidance of an orthoptist and at home after the guidance of the specialist. When performed consistently over several weeks, these exercises can significantly improve the eyes’ ability to converge, reduce symptoms, and enhance reading endurance
Prism glasses
In some more complex cases, prism lenses may be prescribed to reduce the effort needed for the eyes to converge. These lenses help realign the images seen by each eye to reduce visual strain. They are generally used as a supportive measure, often alongside or in preparation for vision therapy.
Lifestyle adjustments and visual hygiene
In both adults and children, making small changes to daily visual habits can go a long way in reducing symptoms:
- Take frequent screen breaks and use the 20-20-20 rule that is every 20 minutes, look at something 20 feet away for 20 seconds
- Ensure proper posture and lighting during near work
- Reduce unnecessary screen time, especially for children
- Encourage outdoor activities, which support healthy visual development
Our specialised team works closely with patients to ensure that they receive practical advice and effective treatment plans tailored to their environment and daily routines.
The importance of early detection
If left undiagnosed, convergence insufficiency can cause years of unnecessary frustration, affecting both academic and personal development. Early detection and treatment can make a profound difference in comfort, concentration, and quality of life
- For children, this can mean being unfairly labelled as inattentive or struggling learners.
- For adults, it may lead to burnout, reduced productivity, and unnecessary discomfort.
By recognising the signs and seeking expert care early on, most individuals can experience substantial improvement and lead more comfortable, visually efficient lives.
Receiving the right treatment for convergence insufficiency
Whether you are a parent concerned about your child’s reading difficulties or an adult experiencing signs of convergence insufficiency, our team is here to help.
At Moorfields Eye Hospital Dubai, our specialised Ophthalmologists and Orthoptists offer personalised assessments and effective treatment plans designed to improve eye coordination, relieve symptoms, and support long-term visual health.
Frequently Asked Questions (FAQs)
Can convergence insufficiency go away on its own?
In some mild or temporary cases, particularly where symptoms are brought on by fatigue or extended near work, convergence insufficiency may seem to improve with rest or lifestyle changes. However, for most individuals, especially children or those with recurring symptoms, it is not likely to resolve on its own. Without targeted intervention, the condition can persist or even worsen over time, impacting day to day activities. Structured vision therapy, led by trained orthoptists, is the most effective way to retrain the eyes and improve vision.
Is it possible to have good vision but still have convergence insufficiency?
Many individuals with 20/20 eyesight still struggle if they have convergence insufficiency. This condition does not relate to how clearly you can see but rather how well your eyes work together when focusing on near tasks. A person may pass a standard vision screening yet experience double vision, eye strain, or difficulty concentrating while reading or using a screen. That is why a comprehensive eye examination, including binocular vision testing, is essential.
At what age can vision therapy begin?
Vision therapy can be effective for both children and adults. In children, therapy typically begins around the age of six or seven, when they are developmentally able to understand instructions and actively participate in exercises. However, earlier assessment can help determine readiness. Teenagers and adults also respond well to therapy, especially when symptoms are impacting school, work, or daily life. The key is a customised programme suited to the patient’s age, attention span, and specific needs.
Is convergence insufficiency linked to dyslexia or ADHD?
While convergence insufficiency (CI) is not considered a direct cause of dyslexia or ADHD, its symptoms can closely mimic those seen in learning or attention disorders. Children with CI may avoid reading, lose their place in text, or struggle to maintain focus on schoolwork, behaviours that overlap with those observed in dyslexia or ADHD. Importantly, CI may be more prevalent in children with specific learning difficulties, making accurate differentiation essential. In some cases, the challenges may stem more from the visual system than from cognitive or behavioural factors. For this reason, a comprehensive eye examination is recommended alongside any neurodevelopmental assessment. Identifying and treating CI can, in certain cases, significantly enhance attention and academic performance
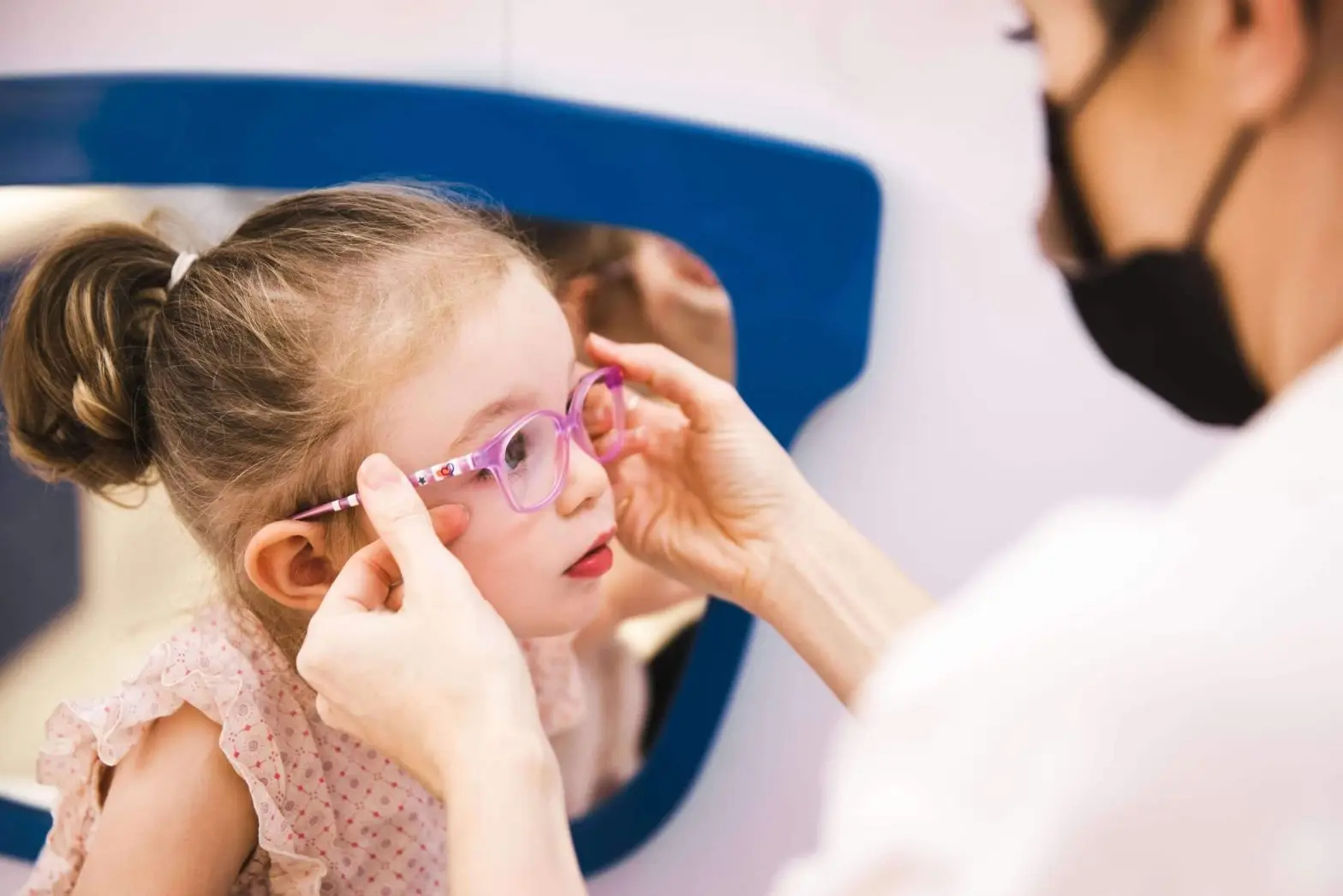
As the new school year begins across the UAE, parents are busy checking off their back-to-school lists: uniforms, supplies, timetables, and lunchboxes. But one important area is often overlooked which is their child’s vision.
Good eyesight is essential not only for reading the board or completing homework but also for building confidence, participating in activities, and staying focused in class. Studies show that up to 80% of classroom learning is visual, which means that undetected vision problems can significantly impact a child’s development and academic progress.
Children may not always realise they have a vision problem, and as a result, they often do not speak up. This makes early detection through regular, comprehensive eye examinations especially important.
At Moorfields Eye Hospital Dubai, we believe that A+ vision builds more than academic success; it builds A+ confidence, A+ independence, and A+ enthusiasm for learning. This back-to-school season, our message is simple: Set their sight for success.
In this blog, three of our leading paediatric ophthalmologists share expert insights on common eye conditions that can affect learning, and what parents can do to ensure their children start the academic year with clear vision and confidence.
Myopia in school aged children
By Dr Imran Jawaid, Consultant Ophthalmologist in Paediatric Ophthalmology and Strabismus Surgery
Myopia, or short-sightedness, is a common vision condition in which distant objects appear blurry, while near objects remain clear. In the classroom, this can mean a child may struggle to read the board, recognise faces from a distance, or participate confidently in lessons. It is one of the most common causes of vision problems in school-aged children and its prevalence is increasing among younger age groups in the UAE.
Rise of myopia
Children today are spending more time on screens and less time outdoors, placing their eyes under prolonged near-vision stress. In Dubai, the rise of indoor digital learning and increased screen time at home has further contributed to this increase. According to the World Health Organization, it is estimated that by 2050, nearly 50% of the global population will be affected by myopia, making early detection and management more important than ever.
Impact on school performance
When a child cannot see clearly at a distance, they may miss out on vital information in class. This can lead to disengagement, academic difficulty, and changes in behaviour. Our aim is to help your child stay focused, participate fully, and perform at their best in the classroom.
Signs of Myopia:
- Difficulty seeing the board
- Sitting too close to the TV or devices
- Complaints of blurry distance vision
- Eye strain and headaches after school
Treatment options:
- Prescription Glasses
- Myopia Control Lenses
- Low-dose Atropine Eye Drops
- Daily Outdoor Play
Effectively managing myopia is not just about improving how a child sees the world, it is about supporting their ability to learn, interact, and grow with confidence. When a child can see clearly, especially at a distance, they are more likely to remain attentive, follow instructions from the board, and feel confident in peer interactions.
Learn more about myopia and its management
Amblyopia (Lazy Eye)
By Dr Salma Yassine, Specialist in Paediatric Ophthalmology and Adult & Paediatric Neuro-ophthalmology
Amblyopia, or lazy eye, is a condition in which the brain favours one eye over the other, causing the weaker eye to develop poor vision. It is because children often rely on their stronger eye, the issue can go undetected without a specialist eye exam.
The impact of Amblyopia on children
Amblyopia reduces depth perception and can make reading, writing, and even physical coordination more difficult. A child with amblyopia may avoid tasks like sports, drawing, or puzzles, not because of lack of interest, but because their vision makes those tasks harder. Over time, this can impact their confidence and academic performance.
Signs of Lazy Eyes:
- Eye turning in or out
- Head tilting
- Clumsiness or lack of interest in fine motor activities
- Reading avoidance or skipping lines
Treatment options:
- Eye Patching
- Corrective Lenses
- Atropine Drops
Amblyopia is most treatable during early childhood. Left untreated, the weaker eye may never develop normal vision, limiting a child’s potential at school and beyond.
By addressing amblyopia early, we help ensure that a child does not face avoidable barriers in school. Supporting healthy vision gives children the clarity and confidence they need to thrive.
Discover more about amblyopia and treatments
Strabismus (Squint)
Strabismus, or squint, is a condition where the eyes do not align properly. Although it may appear cosmetic, it affects how the eyes work together and how the brain processes visual input. In school, it can cause double vision, poor depth perception, and challenges with reading, writing, or sports.
How squints can affect learning and confidence
Children with strabismus may face several challenges in the classroom. They might struggle to copy from the board, avoid reading tasks, or have difficulty catching or tracking moving objects during sports or play. In some cases, the visible misalignment of the eyes can lead to social discomfort, which may affect the child’s confidence and willingness to participate in class activities.
Signs of squints
- Crossed or wandering eyes
- Head tilting
- Eye strain complaints
- Lack of interest in visual tasks
Treatment Options:
- Glasses or Prism Lenses
- Vision Therapy
- Eye Patching (if amblyopia is involved)
- Strabismus Surgery
When properly treated, strabismus can be significantly improved. This can enhance visual function, classroom confidence, and social ease. Children often show increased engagement with reading, copying from the board, and group activities. For some, correcting misalignment also reduces anxiety about how they appear to peers.
Read more about strabismus and available treatments
Set your child’s sight for a Successful School Year
This back-to-school season, ensure your child is not held back by a condition that can be treated or managed with expert care.
At Moorfields Eye Hospital Dubai, we are here to help your child see clearly, learn confidently, and thrive. Our dedicated paediatric department brings together specialised ophthalmologists, orthoptists, and optometrists who work collaboratively to support every child’s visual development. We offer a calm, child-friendly environment and a cooperative approach that puts both the child and their family at ease.
Frequently Asked Questions
At what age should my child first see an eye specialist?
Children should ideally have their first comprehensive eye examination by the age of three. Early checks help detect issues such as refractive errors, lazy eye (amblyopia), or eye alignment problems before they affect a child’s development. An additional exam before starting school ensures their vision is ready for academic activities. After that, regular follow-ups every one to two years are recommended to monitor eye health as they grow.
My child never complains about their eyesight. Could there still be a problem?
Yes. Many children assume their vision is normal and may not express any difficulty. Conditions like amblyopia or strabismus can be present without obvious symptoms. Routine eye examinations are essential to identify issues early — before they begin to impact a child’s learning, behaviour, or confidence in the classroom.
How can I help protect my child’s eyesight as they grow?
Supporting your child’s visual health includes a balance of habits and preventive care. Encourage regular outdoor play (at least 90 minutes daily), limit screen time, and promote breaks during close-up tasks such as reading or device use. A nutritious diet and routine eye check-ups with a specialist are also key to identifying any changes in vision and managing them early.
Will treatments like patching or eye drops affect school routines?
In most cases, no. Treatment plans such as patching or using atropine drops are designed to fit into a child’s daily routine with minimal disruption. Most children continue with school as usual, and teachers can be informed to provide discreet support if needed. Our team works closely with families to make each treatment plan practical and manageable.
Is vision therapy effective for classroom-related challenges?
Yes, particularly for children with amblyopia, eye coordination difficulties, or certain types of strabismus. Vision therapy involves structured exercises that improve how the eyes work together. These activities are often designed to feel like games, making them engaging for children while helping improve reading fluency, focus, and classroom confidence.
How do I know if my child needs glasses?
Some children may show signs like squinting, frequent eye rubbing, holding objects too close, or sitting very near the television. However, not all vision problems are obvious. A comprehensive eye exam is the best way to determine whether your child needs glasses and to ensure their visual development is on track.
Why does my child see an optometrist, orthoptist, and ophthalmologist?
We take a team-based approach to children’s eye care to ensure every child receives a thorough and personalised assessment. Each specialist plays a different but complementary role:
- The optometrist assesses your child’s vision and checks whether glasses are needed.
- The orthoptist examines how the eyes move and work together, particularly in cases of squint (strabismus) or lazy eye (amblyopia).
- The ophthalmologist, a medical doctor, evaluates eye health and provides a final diagnosis, as well as medical or surgical treatment if required.
This collaborative model allows us to build a complete picture of your child’s vision, ensuring nothing is missed and treatment plans are both accurate and effective.
This blog has been authored by Dr.Miguel Morcillo, Consultant Ophthalmologist in Cornea, Cataract and Refractive vision correction surgery.
Living in Dubai often means managing a fast-paced lifestyle, long working hours, and exposure to dusty or humid conditions. For many, glasses and contact lenses can become inconvenient or uncomfortable in such an environment. Laser vision correction offers a life-changing alternative, allowing people to see clearly without depending on corrective eyewear.
Globally, laser eye surgery has one of the highest success rates among elective procedures, with over 95% of patients achieving 20/40 vision or better.
The procedure is considered highly safe when performed by experienced surgeons using modern laser technology. Most individuals return to normal activities within a few days. Millions have safely undergone the procedure worldwide, and interest continues to grow in the UAE.
This guide helps patients understand the options available, who may be a good candidate, and what to expect throughout the journey from consultation to recovery.
Is LASIK Right for You? Laser Vision Correction in Dubai Guide
Laser vision correction is a group of advanced procedures designed to reshape the cornea, the transparent surface at the front of the eye. This improves how light is focused onto the retina (the light-sensitive layer located at the back of the eye), to enhance visual clarity and eliminate the need for glasses or contact lenses.
While many refer to all laser eye surgery as “LASIK,” there are multiple techniques available, each suited to different needs.
Laser vision correction is used to treat the following refractive errors:
- Myopia (short-sightedness): Difficulty seeing distant objects.
- Hypermetropia (long-sightedness): Difficulty seeing near objects.
- Astigmatism: Blurred or distorted vision caused by an irregularly shaped cornea.
- Presbyopia: Age-related near-vision loss, typically after age 40. Correcting presbyopia with Laser vision correction will depend on the surgeon’s recommendation.
Types of Laser Vision Correction (LASIK) in Dubai
There are several advanced laser vision correction techniques available. Each offers specific benefits depending on the patient’s eye health, corneal thickness, and lifestyle needs.
Femtosecond LASIK: This modern technique involves creating a corneal flap using a femtosecond laser instead of a mechanical blade. After the flap is lifted, a laser reshapes the cornea. Benefits include:
- High precision and safety
- Short recovery time (usually within 1–2 days)
- Minimal discomfort
SMILE (Small Incision Lenticule Extraction): SMILE is a minimally invasive procedure that uses a femtosecond laser to create and remove the thin outer layer of the cornea without creating a flap. Benefits include:
- Lower risk of dry eyes
- Quicker healing
- Ideal for active lifestyles
Surface Laser Procedures (PRK or TransPRK): These flapless procedures involve gently removing the outer layer of the cornea before reshaping the underlying corneal tissue and are best suited for:
- Individuals with thin corneas
- Individuals prone to dry eye syndrome
- Recovery may take slightly longer than LASIK and SMILE procedures.
Who is suitable for Laser Vision correction?
Laser eye surgery is life-changing for many, but not everyone is a suitable candidate. A comprehensive eye assessment by a laser vision correction specialist is essential to assess eligibility and type of technique based on individual needs. Ideal candidates are generally:
- 18 years or older
- Have a stable prescription for at least one year
- Have healthy corneas and no major eye conditions such as keratoconus
- Do not have excessively dry eyes
- Are in overall good health
- Understand realistic outcomes of surgery
If laser vision correction is not suitable, alternative options such as implantable lenses (ICL) or refractive lens exchange (RLE) may be recommended.
LASIK preoperative assessment
Before surgery, a comprehensive assessment is performed to determine the best treatment approach and ensure safety. This includes:
- Corneal Topography and Pachymetry: Maps the shape and measure the thickness of the cornea.
- Wavefront Analysis: Detects subtle optical imperfections
- Dry Eye Testing: Assesses tear film quality.
- General Medical and Eye Health History: Assesses overall health and suitability for the procedure.
- Vision Check: Assessment with the optometrist to check vision.
Based on the results, the laser vision correction specialist will advise on the best procedure for your vision and eye health.
What happens during Laser vision correction (LASIK) surgery?
Laser vision correction is a same-day, walk-in procedure that typically takes less than 30 minutes. It is performed using local anaesthetic eye drops, with no need for general anaesthesia. The steps usually include:
- Meet the nurse and complete forms
- Consultation with the ophthalmologist
- Performing the LASIK, PRK, or SMILE technique.
- Completion and post-operative medication and care instructions including follow up appointments
Most patients experience little to no pain. Vision often begins to improve within hours, with significant improvement over the first few days.
Recovery period for Laser Vision Correction (LASIK)
Laser eye surgery is known for its quick recovery time, but proper aftercare is essential. The recovery timeline is as follows:
- First 24–48 hours: Vision may be slightly blurred. Most people can return to work within 1–2 days (depending on the procedure).
- First week: Avoid swimming, strenuous exercise, and rubbing the eyes.
- First month: Attend all follow-up visits to monitor healing.
Eye drops are prescribed to aid healing and prevent infection. Patients are encouraged to rest, avoid makeup, and wear sunglasses when outdoors.
Benefits of Laser Vision Correction (LASIK)?
Improving your vision does more than eliminate the need for glasses or contact lenses. It can transform how you experience everyday life. Reported benefits include:
- Greater freedom in sports, travel, and social activities
- Enhanced self-confidence
- Reduced risk of contact lens-related infections
- Long-term savings on eyewear
For many, waking up and seeing clearly without reaching for glasses is a life-changing moment.
Alternatives to Laser Vision Correction
Some individuals may not be suitable candidates for laser procedures due to eye health, prescription strength, or personal preference. In such cases, alternatives include:
- Implantable Collamer Lenses (ICL): A soft lens is implanted inside the eye, offering permanent vision correction without altering the cornea. Ideal for those with high prescriptions or thin corneas.
- Refractive Lens Exchange (RLE): This involves replacing the natural lens with an artificial intraocular lens, similar to cataract surgery. It is often recommended for individuals over 40 experiencing presbyopia.
Choosing the right facility and specialist
Your eyes are unique, delicate, and deeply linked to how you experience the world. Laser vision correction is a precise medical procedure and its success depends heavily on the skill of the surgeon and the standards of the facility.
When considering where to have your treatment, prioritise clinical expertise, experience, and patient safety. Accredited hospitals with advanced diagnostic tools and strict surgical protocols are best placed to deliver both safe and effective outcomes.
While it may be tempting to compare prices, your vision is not something to compromise. Choosing a trusted, well-established facility ensures peace of mind, not just on the day of surgery, but for years to come.
Investing in your eyesight is an investment in your confidence, independence, and quality of life.
Final thoughts
Laser vision correction offers one of the most effective and rewarding solutions for individuals seeking long-term freedom from glasses or contact lenses. Whether you are navigating busy workdays, active weekends, or just want greater visual independence; this procedure can make a lasting impact.
However, the journey starts with a comprehensive assessment with an expert ophthalmologist specialising in Laser vision correction to ensure you receive safe, personalised recommendations based on your unique eye health
Frequently Asked Questions (FAQs) about Laser Vision Correction (LASIK)
Can laser vision correction treat both eyes on the same day?
Yes, laser vision correction procedures are safely performed on both eyes during the same session. This approach ensures visual balance between the eyes and allows for a more convenient and streamlined recovery. Patients typically appreciate the ability to resume daily activities without delay, and follow-up care is coordinated to support both eyes as they heal simultaneously.
Are there any risks or side effects associated with laser vision correction?
As with any surgical procedure, there are potential risks, although complications are rare when the surgery is performed by experienced specialists using modern technology. Temporary side effects may include dry eyes, mild discomfort, glare, halos around lights, or sensitivity to light, especially at night. These symptoms generally improve within a few weeks. Serious complications are uncommon, especially with thorough preoperative assessments and aftercare.
Is laser vision correction permanent?
Laser vision correction provides long-lasting improvement to correct your current refractive error. However, it does not prevent natural changes in vision that may occur over time due to ageing. For example, most people develop presbyopia in their 40s or 50s, which affects near vision. In such cases, additional treatments or reading glasses may be needed later in life. Moreover, in rare cases where vision changes over time, a follow-up enhancement procedure may be recommended to fine-tune results. That said, many patients enjoy stable, improved distance vision for many years following their procedure.
Can I have laser vision correction if I am pregnant or breastfeeding?
Laser vision correction is not recommended during pregnancy or while breastfeeding. Hormonal fluctuations can affect corneal shape and tear production, which may temporarily alter your vision and lead to inaccurate surgical measurements. It is safer and more effective to wait until your vision has stabilised after breastfeeding, ensuring the most accurate and lasting results.
What should I avoid after laser vision correction surgery?
Post-operative care is important for healing and achieving the best visual outcomes. Patients should avoid the following for at least one week after surgery:
- Swimming in pools, sea water, or hot tubs
- Wearing eye makeup
- Engaging in strenuous exercise or contact sports
- Rubbing or touching the eyes
Wearing protective sunglasses outdoors and using prescribed eye drops are essential during the early recovery period. Your surgeon will provide specific advice based on the type of procedure performed.
Does insurance cover laser vision correction in Dubai?
Laser vision correction is classified as an elective procedure, and as such, it is generally not covered by health insurance plans. However, some providers may offer partial reimbursement or discount agreements. Special rates are also available for holders of Esaad, Fazaa, Saada, Sanad, and Humat Al Watan privilege cards.
This blog has been contributed by Dr. Imran Jawaid, Consultant Ophthalmologist in Paediatric ophthalmology and strabismus surgery
As parents, we do everything possible to support our children’s development and well-being. Vision plays a vital role in a child’s overall growth, supporting learning, movement, and communication from an early age. Yet, one area that can easily be overlooked is eyesight.
Research predicts that conditions such as myopia (short-sightedness) will increase from 27% of the world’s population to 52% by 2050. Moreover, the younger a child is when becoming myopic, the more myopic they will become and the higher the risks of vision-related complications in the future.
Let us take a closer look at why paediatric eye exams in Dubai are so crucial.
Why are regular eye exams essential for children?
Good vision is essential for a child’s development. Unlike adults, young children might not recognise or express that they have a vision problem. This is commonly the case when they have conditions such as near sightedness, farsightedness, and lazy eye. They may assume that everyone sees the way they do, which means they could struggle at school or avoid certain activities without anyone realising the actual cause. Early detection through regular eye exams for children can lead to timely interventions, allowing children to grow, learn, and fully participate in school and everyday life.
What are the most common childhood eye conditions?
Eye conditions can affect children, and early diagnosis can significantly improve treatment outcomes. Some of the most common include:
- Refractive errors: Myopia (short-sightedness), hypermetropia (long-sightedness), and astigmatism.
- Strabismus: Known as a squint or crossed eyes, which can affect depth perception and visual appearance.
- Amblyopia (Lazy Eye): This is a condition in which the brain favours one eye over the other.
- Eye allergies and infections: These cause redness, irritation, or discharge, particularly in younger children.
When should Children have eye exams?
In addition to vision-related checks with your Paediatrician, we recommend that children have their first comprehensive eye exam at around six months old, followed by another at three years of age and then again before starting school. After that, exams every one to two years are advised, or more frequently if your child already has a diagnosed eye condition or significant family history.
With increased exposure to digital screens and close-up work in schools and nurseries, regular eye health monitoring is especially important. Parents should consider booking an exam with a Paediatric eye specialist if their child:
- Squints or tilts their head when looking at objects
- Sits too close to the television or holds books too close
- Struggles with reading or maintaining attention
- Complains of headaches or tired eyes
- Shows signs of clumsiness or poor coordination
- Frequently rubs their eyes or blinks excessively
What happens during a children’s vision screening?
A paediatric eye exam is tailored to suit a child’s age and developmental level. Let us take a closer look at what happens during an exam:
- Meeting Multiple Specialists: Your child will be seen by several specialists, including orthoptists, optometrists, and paediatric ophthalmologists, ensuring a comprehensive review of their eye health.
- Vision testing: Age-appropriate methods to assess how well your child sees with our highly qualified orthoptic team.
- Eye alignment and movement: This exam includes checks to see how well both eyes work together and detect any strabismus (misalignment of the eyes).
- Eye examination: The eyes’ internal structures are examined in detail, sometimes with pupil dilation or using specialist child-friendly imaging if necessary.
What are the treatment options for Children’s eye conditions
When it comes to treating your child’s eye condition, there are both non-surgical and surgical options available to help ensure they receive the best care possible. At Moorfields Eye Hospital Dubai, we provide advanced treatments supported by the latest technology:
Non-Surgical Treatments
- Eyeglasses or contact lenses: The simplest and most common treatments for refractive errors such as myopia, hypermetropia, and astigmatism in children. Eyeglasses are often the first line of treatment to help your child see better, while contact lenses offer an alternative to glasses for active children who might find glasses cumbersome.
- Myopia management includes specialist spectacle lenses, orthokeratology (Ortho-K), eyedrops (low-concentration atropine), and soft contact lenses. We will assess your child’s eyes and work with you to find the most appropriate solution to help slow down their myopia (short-sightedness). There is a wide range of options, and at Moorfields, we have access to the latest technology.
- Patching: Used primarily to treat amblyopia (lazy eye), patching involves covering the stronger eye so the weaker eye is forced to work harder. This method can help improve vision in the affected eye over time.
- Atropine occlusion: Drops can be used in the treatment of lazy eye to blur the vision in the ‘good eye’ to encourage the brain to use the weaker eye, helping to improve the vision.
Surgical Treatments
For conditions such as squint (Strabismus), where non-surgical methods did not treat the condition, surgical intervention may be recommended. This procedure corrects misalignments in the eyes, improving not only eye alignment but also depth perception and overall vision.
Final thoughts
Children’s eye health is crucial to their overall well-being. In a vibrant city like Dubai, where academic and visual demands are high, regular eye exams with children’s eye doctor are one of the most effective ways to support your child’s learning, behaviour, and social development.
If your child has not had an eye exam recently, or if you have noticed any signs of visual difficulty, it is important to get their eyes checked with a paediatric ophthalmologist. Early detection prevents future complications and gives children the best possible start in life.
At Moorfields Eye Hospital Dubai, we are here to help your child see the world clearly—now and for years to come. Let us work together to ensure your child’s vision sets them up for success.
Frequently Asked Questions
Can screen time affect my child’s vision?
Yes, it can. With digital screens becoming a regular part of daily routines, whether for learning or leisure, there has been a noticeable rise in eye strain and early-onset myopia in children (short-sightedness). Staring at screens for prolonged periods, especially up close, can cause discomfort, blurry vision, headaches, and fatigue. It may also encourage poor visual habits, such as holding devices too close to the eyes or forgetting to blink, which affects tear film stability and eye moisture.
To help your child, include techniques like the 20-20-20 rule (taking a 20-second break every 20 minutes to look at something 20 feet away), setting appropriate screen limits, and ensuring balanced visual activities, such as outdoor playtime. These small habits can go a long way in protecting your child’s developing vision.
My child is afraid of doctors—how do you handle nervous children?
We understand that visiting a hospital can be daunting for little ones, especially if it is their first eye exam. That is why our entire paediatric eye care environment is designed to feel calm, safe, and welcoming. Our staff are specially trained in working with children and use gentle, playful, and engaging techniques to build trust.
We allow children to familiarise themselves with the equipment, explain each step in a fun and friendly way, and offer positive reinforcement throughout. Parents are always encouraged to stay by their child’s side during the exam, and we never rush the process. Our goal is not just to complete the assessment but to make it a positive experience your child will be comfortable returning to.
How long does a children’s eye exam take?
A typical comprehensive children’s eye exam takes around 30 to 60 minutes. The exact duration depends on your child’s age, cooperation, and whether additional tests, such as pupil dilation or retinal imaging, are needed. We always aim for a thorough yet efficient experience, balancing accuracy with your child’s comfort.
You will have time to discuss any concerns, and we will ensure your child gets the focused attention they deserve. We recommend allowing a little extra time in your schedule, especially for first-time visits or if your child has specific vision needs.
Can poor vision affect my child’s behaviour or school performance?
Yes, and quite significantly. Many children with vision issues may appear distracted, inattentive, or reluctant to engage in activities like reading or sports, not because of behavioural problems but simply because they are not seeing clearly. This can lead to frustration, low self-esteem, or even being misdiagnosed with learning difficulties.
A simple eye exam can reveal if vision is the underlying cause. With early intervention, whether through glasses, eye exercises, or other treatments, we can make a dramatic difference in your child’s ability to learn and thrive both academically and socially.
Do you offer eye care for children with special needs?
Absolutely. We are proud to offer inclusive and compassionate eye care for children with developmental delays, autism, Down syndrome, and other neurological, behavioural or learning conditions. Our team takes extra time and care to understand each child’s unique needs, tailoring our approach accordingly.
Whether it means adapting communication, simplifying tests, or creating a sensory-friendly environment, we aim to make every child’s experience as smooth and positive as possible. Every child deserves clear vision; we are here to help them achieve it.
How often should children with glasses or existing conditions be seen?
Children who already wear glasses or have known vision conditions should typically be seen every 6 to 12 months, depending on their case. Frequent monitoring allows us to check for prescription changes, ensure treatments are working effectively, and make timely adjustments.
At Moorfields Eye Hospital Dubai, we offer ongoing care and support as your child grows. Regular follow-ups are a key part of safeguarding their long-term visual development.
This blog on Oculoplastic Surgery has been contributed by Dr. Rafic Antonios, Specialist Oculoplastic Surgeon.
Oculoplastic surgery, often known as eyelid surgery, is a specialised field of medicine focusing on the areas around the eyes and the face. This includes the eyelids, orbit (eye socket), and lacrimal (tear) system. The purpose of these procedures ranges from aesthetic enhancements to significant functional improvements, including improvements in vision.
The Interplay Between Oculoplastic Surgery and Vision
Generally, the eyes and the surrounding structures work harmoniously to deliver clear, uninterrupted sight. However, droopy eyelids (ptosis) or eyelid malposition can disrupt this equilibrium, impairing vision. That’s where oculoplastic surgery steps in.
Addressing Common Concerns Through Surgery
Droopy eyelids, a common age-related condition, can obstruct the field of vision, making daily activities like reading or driving challenging. Oculoplastic surgery corrects this by tightening the muscles that lift the eyelid, thereby widening the visual field. Similarly, conditions like entropion (inward-turning eyelid) or ectropion (outward-turning eyelid) can cause discomfort, tear overflow, and blurred vision. Surgery to reposition the eyelid reinstates normalcy, relieving the symptoms and restoring vision clarity.
The Transformative Potential of Oculoplastic Surgery
In conclusion, oculoplastic surgery is not just about cosmetic enhancement. It’s a field aimed at restoring or maintaining the eye’s optimal functionality, significantly impacting vision. While the thought of surgery can seem daunting, understanding its potential benefits can provide reassurance. Consulting with an oculoplastic surgeon could be a transformative step for your vision if you are experiencing vision disruption due to eyelid or surrounding orbital structure issues.
If you are considering oculoplastic surgery in Dubai or want to learn more about how these procedures can enhance your vision and appearance, we are ready to help you by providing personalised care tailored to your unique needs and goals.
Orthoptist Sehar Mann has contributed to this blog on Stages of visual development in Children.
We are all born with blurry vision, and our vision develops in the first 7-8 years of life but is most important when we are babies and toddlers.
Understanding the stages of visual development in babies and toddlers and how they perceive colours can help you provide the correct visual stimulation in their early months of life.
Stages of Visual Development
- The Newborn Stage (0-2 months): Newborn babies can only see objects about 8 to 12 inches from their face – roughly the distance between your face and theirs during feeding or cuddling. They are drawn to high-contrast patterns, like black and white since their eyes are still developing.
- The Infancy Stage (2-4 months): During this period, your baby’s vision starts to improve gradually. They follow moving objects and show interest in colourful toys and pictures. It is normal for their eyes to cross or wander as their muscles strengthen occasionally.
- The Exploratory stage (4-6 months): At 4 to 6 months, babies reach for objects and have better depth perception as they can see more colours more clearly. This is an ideal time to introduce more colourful toys and books with large, bold pictures to stimulate their developing vision.
How Toddlers Perceive Colours
Understanding how toddlers perceive colours can help you create an engaging and stimulating environment for them. Here are some tips to help them:
- High Contrast is Key: In the early months, your baby is drawn to high-contrast colours, such as black and white because they are easier for their developing eyes to distinguish. Consider incorporating these colours into your baby’s nursery decorations or toys.
- The world of Pastels: As babies grow, they will notice more subtle colours like pastels. Soft blues, pinks, and yellows can be soothing and visually appealing for them.
- Vibrant Colours: Babies can see a broader range of colours in the toddler stage. Bright and vibrant colours like red, green, and blue can capture their attention and stimulate their visual development.
Visual Stimulation in the First 6 Months
Visual stimulation is essential for development during the first six months. Here are some simple ways to provide the correct visual experiences:
- Face-to-Face Interaction: Spending quality time making eye contact and talking to your baby can help develop their vision. They love to gaze at your face, and this helps strengthen their visual focus.
- Colourful mobile Toys: Hang a colourful mobile above the crib. The gentle movement and bright colours will intrigue your baby and encourage them to track the objects.
- Picture Books: Choose picture books with large, bold images and vibrant colours. Reading to your baby fosters bonding and enhances their visual recognition skills.
- Tummy Time: Give your baby plenty of tummy time. This helps them develop strong neck and shoulder muscles, which are essential for visual exploration.
- Mirrors: Babies are often fascinated by their reflection. A baby-safe mirror can provide endless entertainment and help with self-recognition.
Watching your toddler’s visual development is an exciting journey that requires your support and engagement. By understanding the stages of visual development and how your baby perceives colours, you can create a stimulating environment that encourages healthy growth and curiosity. Remember, every baby is unique, so enjoy the discovery process together and celebrate each new milestone.
At Moorfields Eye Hospital Dubai, our dedicated paediatric department is staffed with expert ophthalmologists, optometrists, and orthoptists, all passionately dedicated to the eye care needs of children.
Strabismus, commonly called ‘crossed eyes,’ impacts approximately 2% – 4% of children worldwide. This condition results in the misalignment of the eyes, causing them to point in different directions and disrupting binocular vision.
Strabismus is primarily seen in infants and young children and is not just a cosmetic concern. It can significantly impact vision development and depth perception, essential for numerous activities, from catching a ball to crossing a street. When the eyes do not align properly, the brain may start to ignore the image from the eye that is not aligned to prevent seeing double, causing ‘amblyopia,’ also known as a lazy eye.
Emphasising early detection is crucial with strabismus, as the initial years of a child’s life are vital for visual development. Any signs of the condition, such as squinting, tilting the head while looking at objects, or noticeable misalignment of the eyes, should prompt an immediate medical consultation.
The treatment journey for a child with strabismus often involves a team of specialists. An optometrist performs regular eye exams and prescribes glasses if necessary. An orthoptist specialising in strabismus and amblyopia devises personalised eye exercises to improve eye coordination. Lastly, a paediatric eye consultant oversees the child’s treatment, deciding when surgical intervention is necessary and ensuring the various treatments align to maximise visual development and overall quality of life.
In essence, strabismus affects not only the physical appearance but also the functional vision of a child. Therefore, recognising and addressing strabismus in its early stages is crucial for optimal eye health and developmental growth.
If you notice any of the signs or symptoms of Strabismus, please seek care from a specialised ophthalmologist to help your child’s vision develop correctly.
At Moorfields Eye Hospital Dubai, our dedicated paediatric department is staffed with expert ophthalmologists, optometrists, and orthoptists, all passionately dedicated to the eye care needs of children.
This blog on Selective Laser Trabeculoplasty for glaucoma treatment was authored by Dr. Salman Waqar, a Consultant Ophthalmologist in Cataract and Glaucoma Surgery.
Living with glaucoma often means meticulous eye drop management and close intraocular pressure (IOP) monitoring. Thankfully, advancements in eye care, such as Selective Laser Trabeculoplasty (SLT), offer a more refined to manage this condition.
What is SLT?
Selective Laser Trabeculoplasty is a minimally invasive procedure designed to help control glaucoma by decreasing IOP. One of its standout features is the potential to lessen, or in some cases, even eliminate, the dependence on glaucoma eye drops, especially beneficial for those with open-angle glaucoma.
How Does It Work?
Imagine the eye’s drainage system, the trabecular meshwork, as a sink’s drain. Over time, this drain can become less efficient, leading to increased IOP. During this procedure, a precision-targeted laser is applied to this drainage system. Unlike other methods, Selective Laser Trabeculoplasty ensures no thermal damage to the nearby tissue. The treatment encourages the drainage system to work more efficiently by promoting beneficial biological changes within its cells. As the drainage improves, the IOP naturally decreases.
Why Consider SLT?
Selective Laser Trabeculoplasty is revolutionary in its approach. Unlike more aggressive surgeries, it targets only specific cells, ensuring surrounding tissues remain untouched. This selectivity means a less invasive procedure, minimal risks, and quicker recovery times.
However, it’s essential to remember that while it is highly effective, it might not completely negate the need for glaucoma eye drops for all patients. For some, it can notably decrease the amount or frequency of medication, leading to improved comfort and better adherence to treatment.
In Conclusion
Selective Laser Trabeculoplasty is a promising option in glaucoma care. Potentially reducing our reliance on daily eye drops offers a more convenient yet effective way to keep glaucoma in check and safeguard our vision. If you are considering this procedure, discussing it with a glaucoma specialist is recommended to tailor the best care for your eyes.
Cataracts, a common eye condition characterised by clouding of the lens, can affect individuals of all ages. However, people with diabetes are particularly susceptible to developing this condition. In this blog, we will explore the connection between them, understand the underlying mechanisms, and discuss the treatment of cataracts in diabetics.
The connection: Diabetes, a metabolic disorder affecting blood sugar regulation, increases the risk of complications, including eye-related issues such as diabetic retinopathy. Cataracts occur when proteins in the lens clump together, causing clouding and reduced vision. People with diabetes are more likely to develop cataracts at an earlier age and experience faster progression than those without diabetes.
Mechanisms Behind Cataract Formation in Diabetes:
Diabetes can cause cataracts by increasing sugar levels in the body. This can lead to imbalances and changes in the lens structure, making it less transparent. Diabetes can also cause damage to lens proteins, which makes cataracts form faster.
Managing the Risks of Cataracts in Diabetes:
Effective management of cataract risks in individuals with diabetes is crucial. Maintaining stable blood sugar levels through proper diabetes management helps slow cataract progression. In addition, regular eye examinations are essential for early cataract detection. Adopting a healthy lifestyle, including a diet rich in antioxidants, regular exercise, and avoiding smoking, can also reduce the risk of cataracts.
Cataract treatment options for people with diabetes: Surgery is the most effective treatment for cataracts. The procedure involves removing and replacing the clouded lens with an artificial intraocular lens (IOL). People with diabetes must work closely with their doctors to ensure stable blood sugar levels before, during, and after surgery, minimising the risk of complications and optimising visual outcomes.
Understanding the connection between those two conditions and managing the associated risks is crucial for maintaining good eye health. Individuals can effectively navigate this coexisting condition by controlling blood sugar levels, regular eye check-ups, and considering cataract surgery when necessary.