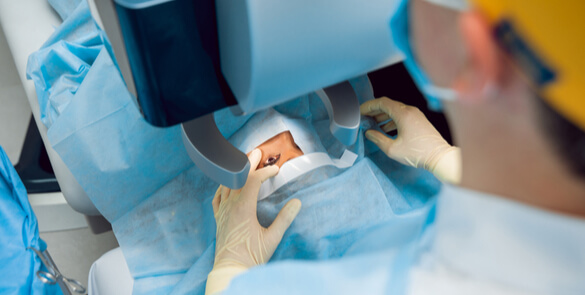
Why do you need a corneal transplant? The cornea is a window of transparent tissue at the front of the eyeball. It allows light to pass into the eye and provides focus so that images can be seen. Various diseases or injury can make the cornea either cloudy or out of shape. This prevents the… Continue reading Corneal Transplantation (PK)
Corneal Transplantation (EK)
Why do you need a corneal transplant? The cornea is a window of transparent tissue at the front of the eyeball. It allows light to pass into the eye and provides focus so that images can be seen. Various diseases or injury can make the cornea either cloudy or out of shape. This prevents the normal passage of light and… Continue reading Corneal Transplantation (EK)
Corneal Transplantation (DALK)
Why do you need a corneal transplant? The cornea is a window of transparent tissue at the front of the eyeball. It allows light to pass into the eye and provides focus so that images can be seen. Various diseases or injury can make the cornea either cloudy or out of shape. This prevents the… Continue reading Corneal Transplantation (DALK)