What is Keratoconus?
This blog on Keratoconus has been contributed by Dr Osama Giledi, Consultant Ophthalmologist, Specialist in Cataract, Cornea and Refractive Vision Correction Surgery
What is Keratoconus?
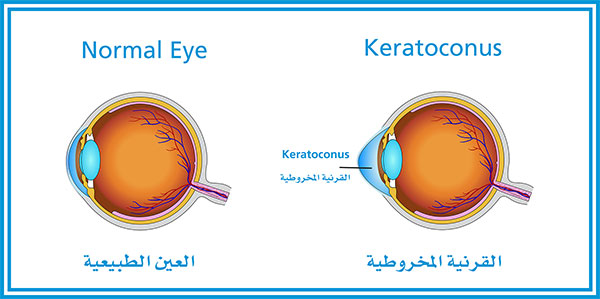
The word Keratoconus comes from two Greek words: kerato (cornea) and konos (cone). Keratoconus is a degenerative disorder of the eye in which the shape of the cornea, which is usually round, is distorted and develops a cone-shaped bulge, resulting in reduced vision. Keratoconus is a relatively common condition. It affects one person in two thousand, occurs around the world and is quite common in the Middle East.
Progression of Keratoconus depends on the patient’s age at the time of onset and the severity of eye rubbing. The earlier the onset, the faster Keratoconus may progress. The condition always affects both eyes and is asymmetric, so one eye may be more affected than the other.
Causes
Keratoconus has many causes, and it results in a cornea that is more elastic than normal and that starts to thin and bulge forward, causing reduced vision and increased astigmatism. It can be inherited, and a chromosomal link has been identified. Keratoconus can be associated with other allergic diseases such as hay fever, eczema and asthma but we are not born with it, and its onset usually happens around puberty. It is strongly associated with eye rubbing, making it progress rapidly. It is also seen in contact lens wearers.
For the best outcome, Keratconus should be detected and treated early. Early detection is possible by generating computerized corneal shape and thickness measurements through corneal topography using advanced technology such as a pentacam machine. If left untreated, Keratoconus could lead to significant visual impairment and blindness.
Treatment
Spectacles
These can provide good vision in the early stages of the condition and usually help to correct myopic astigmatism.
Hard or Scleral Contact Lenses
When spectacles don’t work, rigid contact lenses and Scleral lenses usually provide very good vision if the patient can tolerate them; they should be fitted by a contact lens specialist.
CXL – Corneal Collagen Cross linking with Riboflavin (Vitamin B2)
This technique increases the strength of the cornea and prevents the progress of Keratoconus.
Intracorneal Rings (Intacs & Ferrara)
These rings inserted into the cornea change the shape of the corneal cone, flattening it and making it a more regular and central shape. This will help improve the vision for the majority of patients.
We use it when patients cannot tolerate contact lenses and while the cornea is still clear and the condition is not very advanced. A Femto-second laser is used to create the tunnel and the entry point for the rings, making it a very safe and reliable procedure.
Toric Implantable Contact Lenses
For those with stable Keratoconus and good vision with glasses, Toric Implantable Contact Lenses are generally used (sometimes after stabilizing the Keratoconus with corneal cross linkage) to improve corneal shape with an intracorneal ring or with very limited therapeutic Excimer laser correction. The Toric ICL can eliminate the need for optical aids altogether and, in some patients, results in improved vision and balance between the two eyes.
Phototherapeutic Keratectomy (PTK)
Keratoconus patients are not candidates for Lasik or normal laser correction. However, some patients benefit from limited excimer laser correction to improve the surface irregularity of the cornea when
contact lenses cannot be tolerated. PTK is always combined with corneal cross-linkage, undertaken during the same procedure or afterwards.
Corneal Transplants
Corneal Transplants are used in the advanced stages of Keratoconus, when there is corneal scarring. The procedure is either a partial thickness (Deep Anterior Lamellar Keratoplasty = DALK) or full thickness graft (Penetrating Keratoplasty = PK). The need for corneal grafts is declining because of the increasing success in the early diagnosis of Keratoconus and the effectiveness of corneal cross linkage to stabilize the condition, so Keratoconus generally does not reach the advanced stage.